Welcome to your MESSA 3-Tier Rx plan
Your MESSA 3-Tier Rx plan is available with our MESSA ABC and MESSA Choices medical plans. It offers a mix of copays and coinsurance, making it easy to budget for your Rx expenses.
This page explains how it works, how to check your coverage and where to go if you have questions.
Check your Rx coverage
If you have questions about your coverage for a particular medication, it’s easy to get answers.
Check your Optum Rx portal
- Log in to your MyMESSA member account.
- Under Benefits in the top navigation, select “Optum Rx home delivery.”
- Once you’re logged into your Optum Rx portal, select “Drug list tool” under Member Tools.
- Search for your medication to see coverage details and get cost estimates for home delivery and other options.
Contact MESSA
- Call our Member Service Center at 800-336-0013.
- Log in to your MyMESSA member account to live chat with us or send a secure message.
Don’t have a MyMESSA account? It takes just a few minutes to set one up.
How 3-Tier Rx works
MESSA’s 3-Tier Rx plan includes several money-saving features including:
- Prior authorization
- Quantity limits
- Step therapy
3-Tier Rx works differently depending on whether you have an ABC medical plan or a Choices medical plan. Get the details for each plan below.
MESSA ABC with 3-Tier Rx
With a MESSA ABC plan, you pay the full cost of your prescriptions until your deductible is fully paid. After you meet your deductible, you are responsible for prescription copays or coinsurance until you reach your out-of-pocket maximum.
| Types of medications | Up to 34-day supply | 90-day supply |
|---|---|---|
| An expanded list of preventive medications are covered 100% with no deductible. See the list. | No cost to you | No cost to you |
| After your deductible is met, the following costs apply: | ||
| Generic drugs Members pay the lowest copay for generics, making them the most cost-effective option for treatment. |
$10 copayment | $25 copayment |
| Preferred brand-name drugs These drugs are more expensive than generics. |
20% coinsurance $40 minimum to $80 maximum | 20% coinsurance $100 minimum to $200 maximum |
| Nonpreferred brand-name drugs Includes brand-name drugs for which there’s either a generic alternative or a more cost-effective, preferred brand-name drug available. |
20% coinsurance $60 minimum to $100 maximum | 20% coinsurance $150 minimum to $250 maximum |
Additional resources
MESSA Choices with 3-Tier Rx
With a Choices plan, you pay copays or coinsurance depending on the medication until you reach your prescription out-of-pocket maximum.
| Types of medications | Up to 34-day supply | 90-day supply |
|---|---|---|
| Specific preventive medications mandated by federal law are covered 100%. | No cost to you | No cost to you |
| Generic drugs Members pay the lowest copay for generics, making them the most cost-effective option for treatment. |
$10 copayment | $25 copayment |
| Preferred brand-name drugs These drugs are more expensive than generics. |
20% coinsurance $40 minimum to $80 maximum |
20% coinsurance $100 minimum to $200 maximum |
| Nonpreferred brand-name drugs Includes brand-name drugs for which there’s either a generic alternative or a more cost-effective, preferred brand-name drug available. |
20% coinsurance $60 minimum to $100 maximum |
20% coinsurance $150 minimum to $250 maximum |
Additional resources
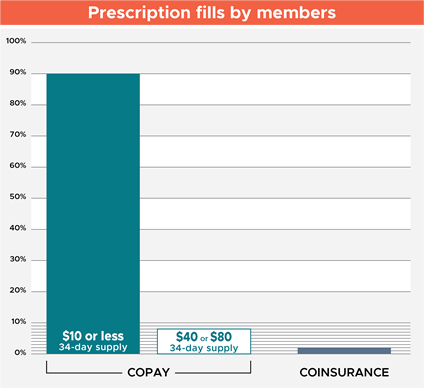
Copay vs. Coinsurance
A copay is a fixed amount you pay for a medication. Coinsurance is a percentage you pay based on the cost of the medication, with a set maximum amount.
More than 98% of prescriptions filled by MESSA members have flat-dollar copays of $10, $40 or $80.
Overall, more than 90% of drugs have a copay of just $10.
Specialty medications
Specialty medications are handled separately. Specialty drugs must be obtained by mail through Walgreens Specialty Pharmacy or select Walgreens retail pharmacies. If you obtain specialty medications from any other provider, you may be responsible for the total cost.
The initial quantity of select specialty drugs may be limited, and your cost will be reduced accordingly. Additional fills for specialty drugs are limited to a 30-day supply.
Still have questions?
We’re happy to help.
- Call MESSA’s Member Service Center at 800-336-0013 to speak with a friendly knowledgeable member service specialist.
- Send us a secure message or live chat with a member of our team through your MyMESSA member account.
Helpful prescription plan terminology
Some medications have prior authorization, step therapy or quantity limit requirements. These are all tools to help keep costs down while making sure you get the medication and treatment you need.
- Prior authorization. To ensure compliance with FDA-approved safe prescribing guidelines, certain drugs require prior authorization before MESSA will cover them. For these drugs, your doctor must submit proper documentation supporting the need for the prescription.
- Step therapy. Drugs subject to step therapy require previous treatment with one or more preferred drugs before coverage is approved. If your prescribed drug does not meet the step therapy criteria, it may not be covered.
- Quantity limits. Our quantity limit program encourages safe medication use. Certain medications are available in limited quantities based on the FDA’s approved dosing guidelines.





